Associates in Women's Health
1046 North Monroe Street
Monroe, MI 48161 US
Monday:
8:00 am - 5:30 pm
Tuesday:
8:00 am - 4:30 pm
Wednesday:
10:00 am - 6:00 pm
Thursday:
8:00 am - 7:00 pm
Friday:
8:00 am - 3:00 pm
Saturday:
Closed
Sunday:
Closed
My Blog
-
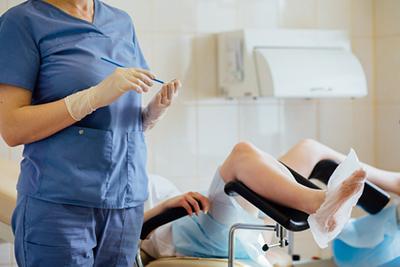
Reproductive Health Screenings: Importance and Frequency
posted: Apr. 17, 2024.

-
Pelvic Floor Health: Exercises and Strategies for Preventing Incontinence
posted: Apr. 01, 2024.

-
What Are Common Signs of a Hormonal Imbalance in Women?
posted: Mar. 15, 2024.

-
When To See an OBGYN
posted: Mar. 01, 2024.

-
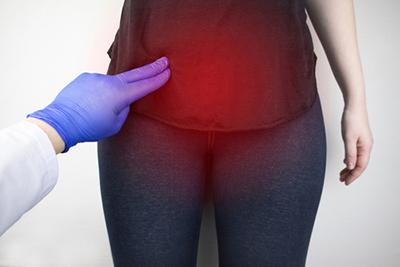
Signs of Abnormal Uterine Bleeding
posted: Feb. 26, 2024.
-
What Does an OBGYN Do?
posted: Feb. 13, 2024.

-
Abnormal Uterine Bleeding FAQs
posted: Jan. 07, 2024.

-
What To Know About Menopause
posted: Jan. 01, 2024.

-
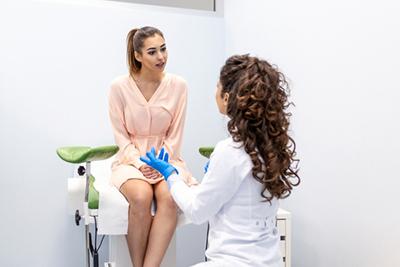
Well Women Care
posted: Dec. 11, 2023.
-
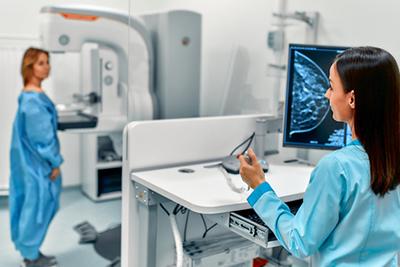
Breast Cancer and Breast Exams
posted: Dec. 01, 2023.
-
The Importance of Regular Check-ups: Exploring the Benefits of OBGYN Visits
posted: Nov. 07, 2023.

-
Understanding the Role of an OBGYN: What They Do and Why It Matters
posted: Nov. 01, 2023.
-
Age-Related Gynecological Issues
posted: Oct. 13, 2023.
-
Infertility Treatments and Options
posted: Oct. 05, 2023.

-
Benefits of Having an OBGYN
posted: Sep. 12, 2023.
-
What To Know About Irregular Bleeding
posted: Sep. 01, 2023.

Our Location
Find us on the map
Office Hours
Our Regular Schedule
Monday:
8:00 am-5:30 pm
Tuesday:
8:00 am-4:30 pm
Wednesday:
10:00 am-6:00 pm
Thursday:
8:00 am-7:00 pm
Friday:
8:00 am-3:00 pm
Saturday:
Closed
Sunday:
Closed